Telemedicine malpractice insurance
Telemedicine is a service that makes it easier for healthcare professionals to provide medical care, but it might also increase the risk of a misdiagnosis or patient complaint. That's why it’s important to get the right medical professional liability insurance policy as part of your risk management plan.
What is telemedicine?
Telemedicine allows medical providers and patients to communicate over the phone or video calls, rather than having an in-person diagnosis at an office. This is especially useful when patients are unable to come in for an in-person office visit.
Telemedicine services can be used for a number of healthcare services such as follow-up visits, preventive care, and managing the patient’s ongoing medical conditions.
The use of telemedicine coverage and virtual care became prevalent during the COVID-19 pandemic, with over a third (37%) of adults reporting that they have used telemedicine services in 2021.
This trend is expected to grow. In fact, the worldwide telehealth industry is expected to reach over $450 billion by 2030.
Is telemedicine covered by medical malpractice insurance?
Medical malpractice insurance, also known as professional liability insurance or errors and omissions insurance, protects healthcare professionals against claims of professional negligence and mistakes, including the care you provide through telemedicine.
Malpractice insurance is often required by state law for those in the medical field. You may also have to be licensed in a particular state in order to provide telehealth services there.
Check with your state licensing board to make sure you comply with the law. Many states have privacy laws specifically for telehealth visits, and the ones that don’t could issue new requirements in the future to address this growing trend.
It’s also a good idea to check with your insurance company to be sure you’re covered for telehealth visits and if they have any requirements for these services.
You’ll also need to make sure you don’t violate any Health Insurance Portability and Accountability (HIPAA) regulations, especially if you’re unfamiliar with telehealth platforms and methods.
The Office of the National Coordinator for Health Information Technology (ONC) has more information on staying HIPAA compliant on their “Know the risks [PDF]” page.
Malpractice insurance is often required by state law for those in the medical field.
How do I get telehealth malpractice insurance?
It's easy to get free quotes for medical malpractice insurance with Insureon. We'll ask you basic facts about your business to help you find coverage that matches your unique risks and meets the requirements in your state.
Contact our dedicated medical malpractice insurance specialist to get started.
What our customers are saying
What does telemedicine malpractice insurance cover?
A malpractice insurance policy covers issues such as:
- The misdiagnosis of a patient
- Treatment errors
- Improper medications or dosage
- Misreading or ignoring lab results
Telehealth medical services carry the same malpractice risks, but with an increased exposure to:
- HIPAA and Health Information Technology for Economic and Clinical Health (HITECH) violations
- Violations of state law (such as offering treatment across state borders)
- Failing to meet the required standards of care
The HIPAA Security Rule stipulates that physicians use “reasonable and appropriate safeguards” to keep electronic protected health information (ePHI) secure. As well as the HIPAA Journal [PDF], which reports texting, Skype, and email do not meet the Security Rule’s requirements.
Stipulations by HIPAA mandate that:
- Only authorized users can access ePHI
- Medical providers must have a secure communication method to protect ePHI
- Any communications containing ePHI should be monitored to prevent accidental or malicious breaches
Depending on the laws in your state, you might also need to inform your patients of the risks and limitations of telehealth visits and receive either written or verbal approval from them.

Who needs telehealth medical malpractice coverage?
Any healthcare professional who’s responsible for patient care and privacy should have malpractice insurance, with sufficient telehealth coverage if they provide any patient services over the phone or online.
This is especially true since the COVID-19 pandemic, as medical providers have expanded their telehealth coverage to treat patients who were reluctant or unable to make an in-office visit.
Healthcare professionals who may need medical malpractice coverage more than than others include:
Physicians
A physician might misdiagnose a patient over a video call. Even if the misdiagnosis was based on a patient’s inability to accurately describe their condition, the doctor could still face a malpractice claim.
Nurses
Nurses often face the same risks as doctors. If they misdiagnose a patient or provide a wrong treatment plan, they could be at risk of a malpractice lawsuit. That includes registered nurses, nurse practitioners, nurse anesthetists, midwives, and other nursing professionals.
Physician's assistants
Physician’s assistants often deal with confidential information and patient care. They may be responsible for managing a doctor’s telehealth services and interacting with patients. All of this puts them at risk of a malpractice lawsuit from a disgruntled patient.
Therapists
Therapists who offer video therapy or teletherapy services can be vulnerable to claims of negligence. For instance, a client might be seeing a virtual therapist to help their battles with addiction. If that client relapses, they could sue the counselor by claiming that they failed to prevent the relapse.
Top healthcare and therapy/counseling professionals we insure
Don't see your profession? Don't worry. We insure most businesses.
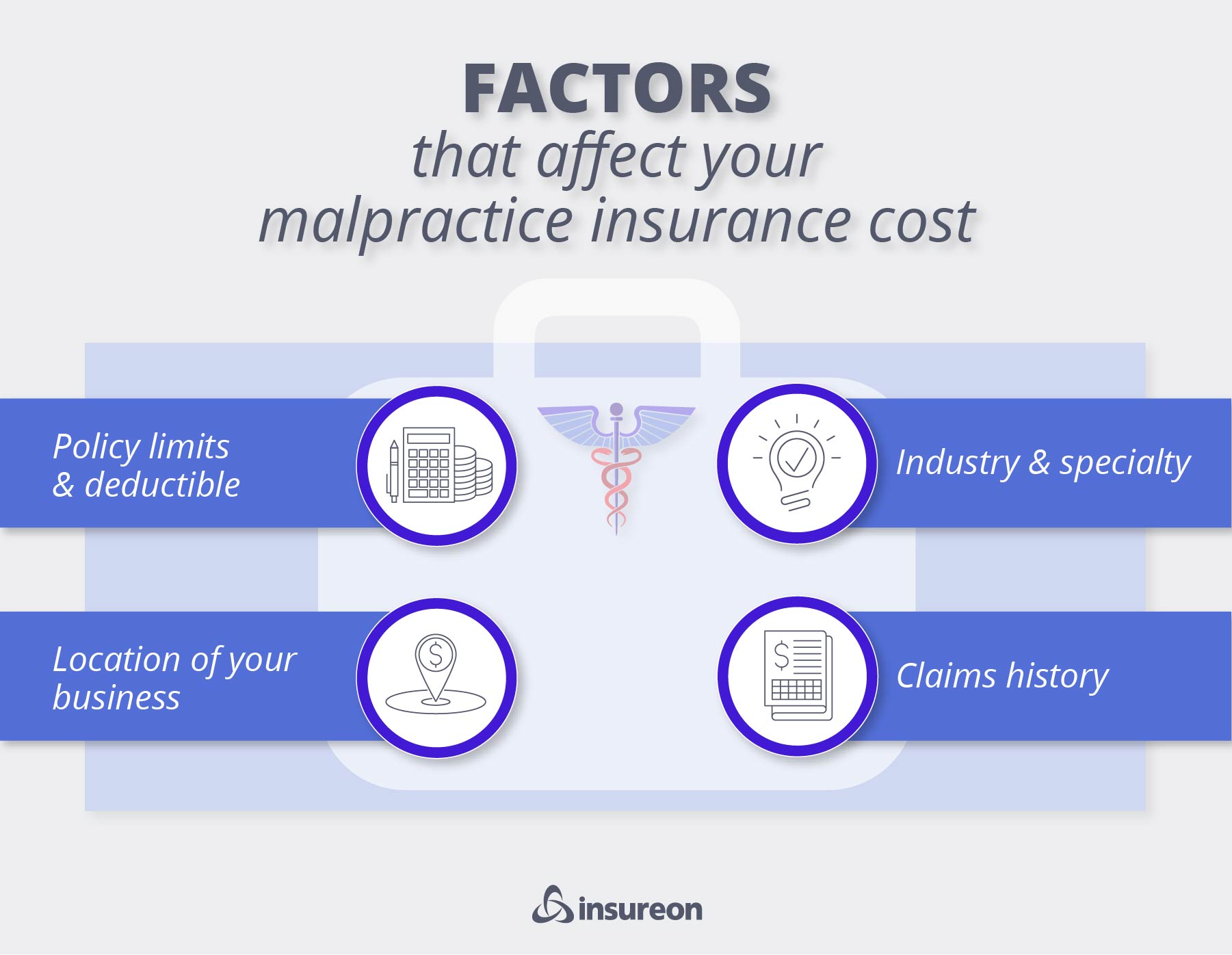
How much does telemedicine malpractice insurance coverage cost?

Your premium for telemedicine malpractice insurance depends on several factors, such as the risks of your profession.
Other factors that affect malpractice insurance costs include:
- Your location
- Your policy limits and deductible
- Your liability claims history
- Any malpractice lawsuits you’ve faced
How does telemedicine malpractice coverage differ from other types of business insurance?
While you might already have general liability insurance and cyber liability insurance, these policies cover different things than a medical liability policy.
General liability insurance covers common third-party risks, such as slip-and-fall accidents at your office. It is often the first type of insurance small business owners get as it's often required to attain a commercial lease and client contracts.
Cyber liability insurance offers financial protection against the cost of data breaches and cyberattacks.

General liability and professional liability insurance both protect against common small business liabilities, but cover two different types of lawsuits. You may need to purchase one or both policies depending on your risks.
Find free quotes and buy online with Insureon
Are you ready to safeguard your business with malpractice insurance? You can call our dedicated medical malpractice insurance agent at (312) 854-2919 to get started today.